Conventional medicine
Quantify the disorder. Identify apnea, insomnia, restless legs, or circadian shift. Treat apnea with CPAP / oral appliance. Treat insomnia with CBT-I or Rx. Refer to sleep medicine if refractory.
Circadian-first / behavioral
Most chronic poor sleep traces to broken circadian inputs and conditioned arousal in bed. Fix the inputs in the right order, and pharmacology rarely needs to enter.
History, STOP-BANG (apnea risk), ISI (insomnia severity), Epworth (daytime sleepiness). Rule out depression, thyroid, anemia, meds.
Log bed time, wake time, sleep latency, awakenings, caffeine, alcohol, meals, exercise, screen cutoff, wake mood. Use STOP-BANG online for apnea risk.
Home sleep apnea test (HSAT) for high apnea pretest probability. Polysomnography (PSG) for atypical cases, complex insomnia, suspected parasomnia.
Morning sunlight 5–10 min within 1 hr of waking. Dim ambient light after sunset. No bright overhead light or screens 2 hrs pre-bed. Fixed wake time ± 30 min, weekends included.
CPAP titration + 90-day mask trial for moderate-severe apnea. Custom mandibular advancement device for mild-moderate or CPAP-intolerant. CBT-I as first-line insomnia.
Bedroom 65–68°F. Warm shower 90 min pre-bed (drops core temp). Cap caffeine at 200mg, by noon. No alcohol within 3 hrs of bed. Last meal 3 hrs out.
Refractory cases. Titrate CPAP pressure. Consider hypoglossal nerve stim (Inspire) for select apnea. Pharmacotherapy: DORA (suvorexant, lemborexant), melatonin, low-dose doxepin.
Bed = sleep only. Out of bed if not asleep in 20 min. No daytime naps. Sleep restriction (compress sleep window to actual sleep time, then expand). Cognitive reframing of awake-in-bed worry.
Septoplasty / turbinate reduction / UPPP for anatomical apnea. MMA (maxillomandibular advancement) for severe. Hypoglossal nerve stim implant for CPAP-failure.
Fixed wake time. Morning light. Caffeine before noon. 3-hr alcohol buffer. Cool dark bedroom. Movement daily. Reassess if Epworth >10 or snoring loud → sleep study.
Every step has a price.
Here’s what we found.
We called clinics across Austin and pulled cash-pay quotes. Click any tile for the full provider list, phone numbers, and last-verified dates.
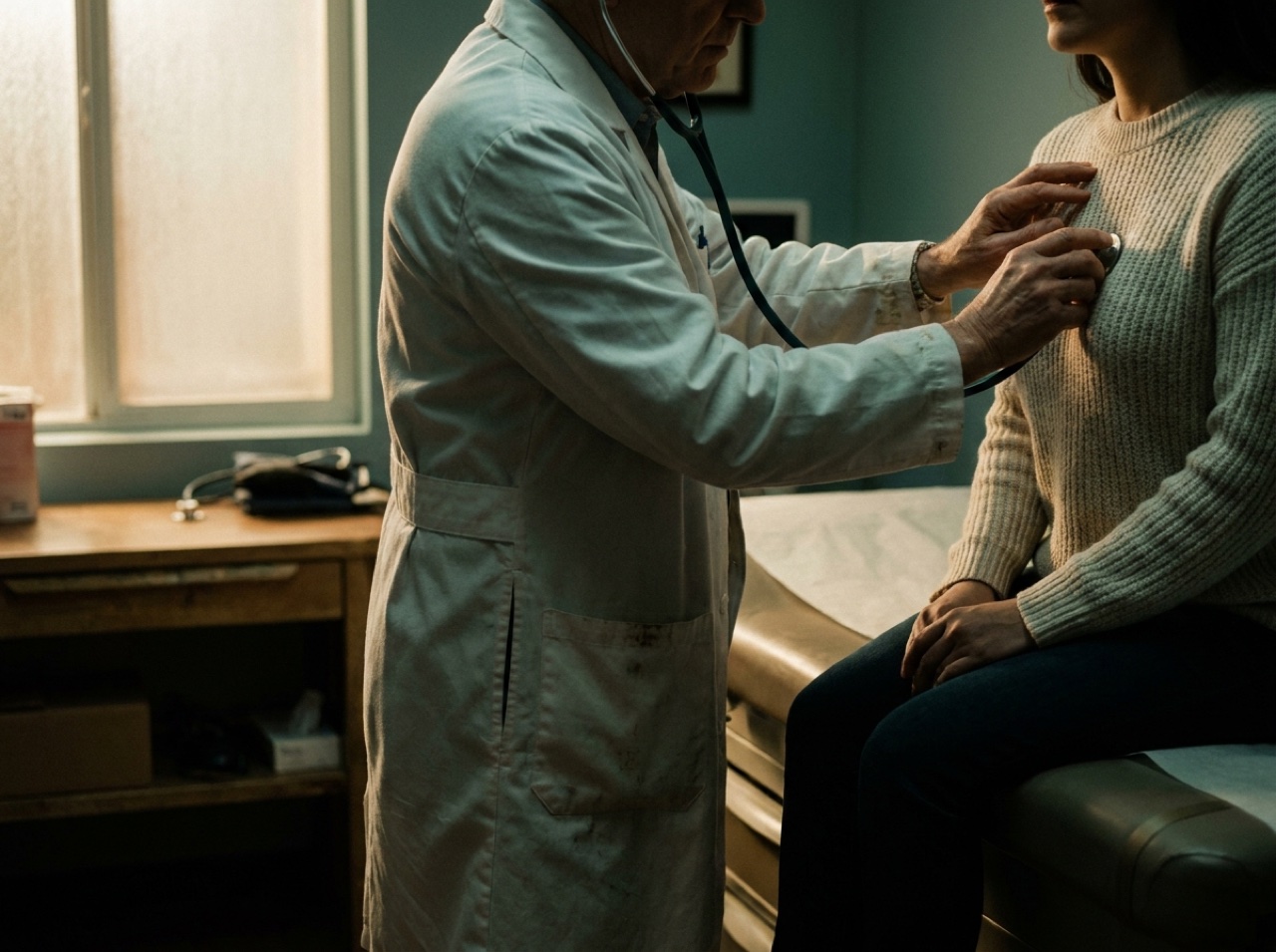






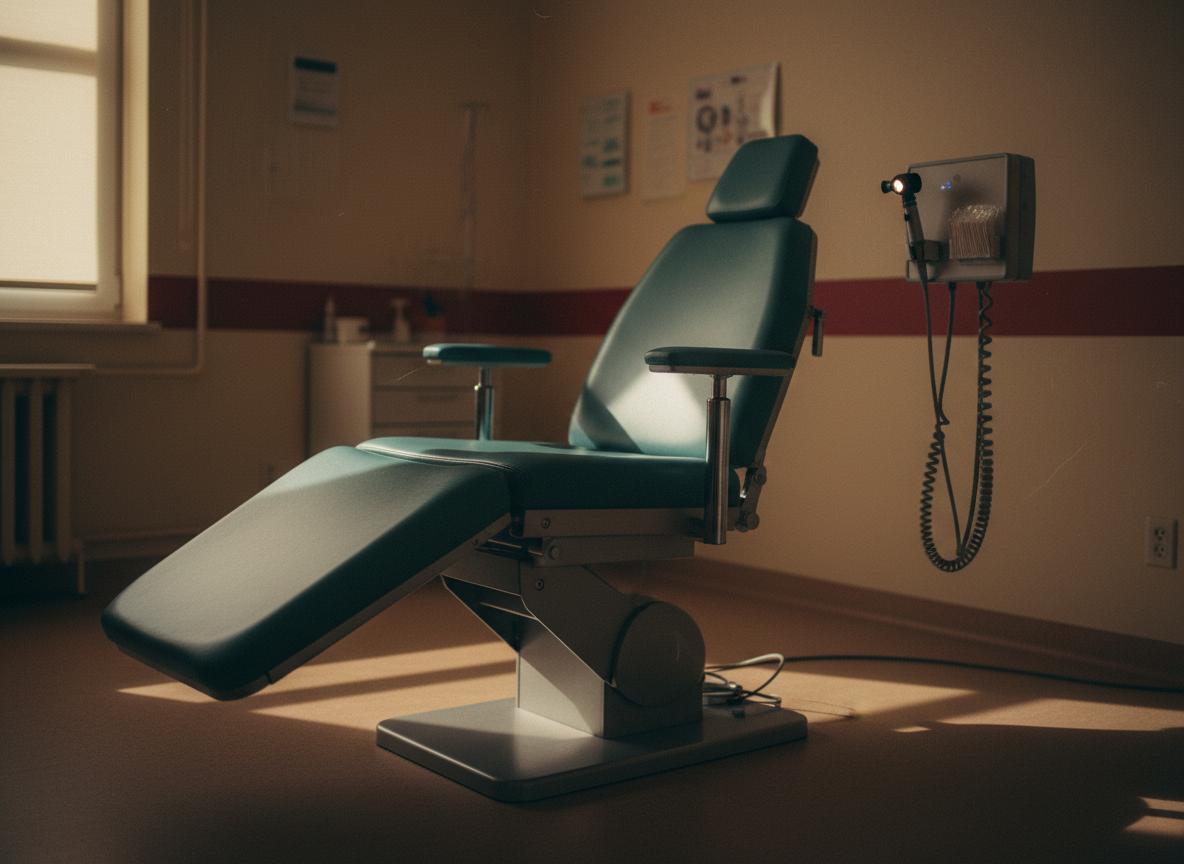
Who built
track B.
Researchers and clinicians on the behavioral side of sleep. CBT-I sits in both tracks because it’s evidence-based AND non-pharmacological.

"Sleep is the single most effective thing we can do to reset our brain and body health every day." Fixed schedule, no alcohol within 3 hrs.

Morning sun + low light at night = circadian gold standard. Temperature drops trigger sleep onset.

Chronotype-matched routines. Most insomnia is conditioned arousal in bed; stimulus control fixes it.

Sleep is non-negotiable for healthspan. Track HRV + sleep latency. Treat apnea aggressively.
- AASM Clinical Practice GuidelinesSpecialty body
- Annals · CBT-I vs hypnotics meta-analysisMeta-analysis
- Cochrane · CPAP for OSASystematic review
- Matthew Walker · Why We SleepUC Berkeley sleep researcher
- Andrew Huberman · Huberman LabStanford neuroscientist
- Dr. Michael Breus · thesleepdoctor.comClinical sleep psychologist
- Peter Attia · The DriveMD · longevity-focused